Life Coaching Interview Ques #2_July05 return to question one Link to Background information
|
The History
|
|
Navigational Short Cuts:
|
Preserving
the health of already healthy mothers
and babies is the
primary
purpose of maternity care
The gold standard for maternity care is the same the world over and through out history, it is the same in every language -- the goal is and will remain the practical wellbeing of the mothers and babies it services.
Midwifery as an organized body of knowledge and set of technical skills preceded the modern discipline of medicine by more than 5,000 years. Historically childbearing women themselves were the best (and only!) source of information about the biology and physiology of pregnancy and normal childbirth. For thousands and thousands of years, women gave birth normally with the support of their extended families and the help of experienced older women. For healthy women in safe surroundings, pregnancy and birth was generally successful for them and their babies. We know this statement is true because the human species has survived (and in fact, thrived) into the 21st century. Anyone alive in the 21st century is a direct descendent of women who were successful at giving birth normally, without the need for forceps or cesarean surgery.
Eve 2.0 ~ Nature's program for normal birth
From the get-go of the human species, older experienced women always helped younger, inexperienced women during the hours of labor and during the moments of birth. This also included caring for the new mother for some days afterwards, as she learned to breastfeed and take care of her new baby. This type of experienced assistance (Eve 2.0!) eventually become known as “midwifery” . Those women caregivers who developed specialized skills in managing childbirth and dealing with the needs of new mothers and babies were known as ‘midwives’. In the old world language of England, the word ‘mid’ meant “with” and the word ‘wife’ referred to “woman”. Thus a ‘midwife’ was someone who was ‘with woman’ during the events of childbearing.
“The practice of midwifery dates back to the beginning of human life in this world. At this supreme moment of motherhood it is probable that some assistance has always been required and given. Its history runs parallel with the history of the people, and its functions antedate any record we have of medicine as an applied process. To deny its right to exist as a calling is to take issue with the eternal verities of life.” Dr. Josephine Baker, M.D. 1911-G, page# 232
The first record of midwifery as an established discipline can be found in the hieroglyphics of ancient Egypt in 3,000 BC. The first mention of midwives in Western culture (perhaps prophetically) is a story in the Old Testament of political intrigue and civil disobedience. The book of Exodus records the clash between the Egyptian Pharaoh, who ordered his midwives to kill all the first-born sons of the enslaved Hebrew population. The Egyptian midwives, at great risk to their own lives, declined to carry out such orders. When these midwives were called before the Pharaoh to explain why they did not do as directed, they answered that the Hebrew women, unlike the Egyptian women, were “lively upon the birth stool” and delivered before the midwives arrived.
“The practice of midwifery is as old as the human race. Its history runs parallel with the history of the people and its functions antedate any record we have of medicine as an applied science. Midwives, as a class, were recognized in history from early Egyptian times.” Dr. Hardin, M.D.1925-A; p. 347
During the first 5,000 years of recorded history, the discipline of midwifery was empirically-based and organized around meeting the practical needs of laboring women. These universal needs are primarily psychological, emotional, and social. The care of midwives included ‘patience with nature’, the right use of gravity and a commitment not to disturb the natural process. Again, we must accept as fact that this was a successful strategy, as the human species has survived and thrived under the care of their midwives. No medical drug or devise, no surgical instrument or procedure ever developed by medical science has been able to make birth better or safer in healthy women with normal pregnancies than spontaneous labor and normal birth attended by an experienced birth attendant.
These protective
methods are what we now refer to as
“physiological management” –
that is,
“…in
accord with, or characteristic of, the normal functioning of a
living organism”.
The classic principles of physiological management include a basic trust in biology and support for the normal process of labor and birth. It is a tradition that restricts the use of interventions to abnormal situations only. This non-interventive approach recognizes the mother’s need for physical and psychological privacy and to feel safe from unwanted intrusions and the prying eyes of strangers. Physiologic care encourages the mother to walk around at will and to be upright and mobile during both labor and birth. It also includes continuity of care by individuals known to the mother, one-on-one social and emotional support, non-drug methods of pain relief (such as movement, touch and warm water), patience, and the right use of gravity.
“...that trained midwives surpass the record of physicians in normal deliveries has been ascribed to several factors. Chief among these is the fact that the circumstances of modern practice induce many physicians to employ procedures which are calculated to hasten delivery, but which sometimes result in harm to mother and child. On her part, the midwife is not permitted to and does not employ such procedures. She waits patiently and lets nature take its course." [1931 Testimony on midwifery care, White House Conference on Child Health and Protection by the Committee on Prenatal and Maternal Care]
|
Gravity – What a concept! |
|
Even though traditional midwives had no formal training in the science-based study of anatomy as we think of it today, they had ample opportunity to observe that childbearing women, when left to their own devices, almost universally chose to be mobile during labor and to assume some form of upright position during the birth of the baby. The right use of gravity naturally stimulates effective uterine contractions, the dilatation of the cervix and the decent of the baby through the bony pelvis. On the rare occasions that circumstances required the mother to lie down, midwives also noted that the labor was much slower and the mother had to push longer and harder to get the baby out. Sometimes she wasn’t able to deliver unless or until she got back up into a gravity-friendly position.
The childbearing pelvis – that is, the internal bones that the baby must pass through -- normally creates a hollow space shaped like a lower-case letter “j”. Most people erroneously think of the birth canal as a straight chute (lower-case ‘l’), going straight down thru the lower half of the mother’s body; in other words, if the mother was lying down and you were watching her from the side, her baby would pass through the pelvis and out of her body the same way a train comes out of a tunnel – a straight cylindrical object passing thru a straight cylindrical container.
But this idea is not anatomically correct.
Imagine instead that you are looking at an upright pregnant woman from the side as she labors and gives birth while still in an upright posture. If you had x-ray vision, you would see that the long stem of the ‘j’ tracks with the mother’s lower spine and the curved foot of the letter bends forward to track with the lower half of the birth canal. What this means is the pelvic outlet -- last 1/3 of the journey – bends at a 60-degree angle, which requires that the baby to go around a corner and emerge into the world going forward (into its mother’s arms!) instead of straight down towards the floor, where it would be hard to reach and might be injured as it fell to the ground. Not doubt this “frontal delivery” is an important survival characteristic, as 99.99% of human history predates hospital obstetrics, which meant it was the mother herself who was responsible for ‘catching’ her baby.
Were you to look down into the pelvis from the top, you would notice that the big triangle-shaped bone of the lower spine -- the sacrum and coccyx -- encroaches into the pelvic outlet about an inch or so. In this regard, the pelvis is like a hollow bowl with smooth walls on three sides but slightly bent in on the fourth side, making it impossible for anything that is the same size and shape as its circumference to pass through.
| The sacrum (at left) the public bone (at right) and the relationship of the baby's head to these bones, as it travels down thru the birth canal. The baby's head makes a 60 degree arc down thru the birth canal and rotates under the pubic bone. When the mother is upright, |
|
However, in the second stage of labor, after the baby is squeezed out of the uterus thru the cervix and starts its trek down into the birth canal, you would see something remarkable happen. In pregnancy the sacrum and coccyx are movable and able to be pressed back out of the way by the baby’s head, as it descends deeper into the birth canal and gets closer and closer to being born. In addition, the hormones of pregnancy soften the cartilage that hold the two sides of the pubic bone together, so this pelvic joint become unusually elastic. This permits the pelvis to also stretch and widen side to side, which can give the baby an extra 1-2 centimeters of room to negotiate its passage into the world.
 |
|
|
For a laboring mother, lying down is an anti-gravitational position that can reduce the pelvic size by almost a third, while simultaneously requiring the mother to push her baby up hill, and around a 60-degree bend. Not only does this require that she defy gravity, but she must do this with the doorway partially blocked, reducing the aperture of the pelvis. When the mother is bearing her own weight on her lower spine, such as lying back with her legs held up in stirrups, the sacrum cannot move back out of the baby's way.
If the baby is small or the mother’s pelvis is big,
the normal forces of labor and extra effort by the mother can overcome this
impediment. However, when the mother is on her back, the baby must
still emerge at an angle heading upwards, towards the ceiling. Obviously this
is a lot harder and takes a lot longer than it would if gravity were used to
benefit mother and baby. If the mother has been anesthetized, it
may require the use of obstetrical forceps to extract the baby.
Unfortunately, if the baby is unusually big or the mother's pelvis unusually
small, the baby can get stuck. This describes the ‘obstructed labor’ of Old
World fame. In this case the baby would eventually die after 4 to 6 days of
useless labor. In modern life, a Cesarean section would be done after some hours
of effective pushing without any progress.
|
|
This is graphic of a mother giving birth without the added benefit of gravity, while lying on her back. The baby must first negotiate its way under the pubic bone by rotating its head from sideways to an up / down orientation. Then the crown of the baby's head |
Evidence-based Maternity Care for the
21st
Century
The scientific basis for physiological management of pregnancy and normal childbirth is supported by a consensus of the scientific literature. Physiological management is actually protective for both mothers and babies, reducing the episiotomy / operative delivery rate (and its associated complications), from approximately 70% to approximately 5% with an identical, or even slightly reduced perinatal mortality rate.
The following are the core principles for a national, evidence-based maternity care policy:
(1) Preserving the health of already healthy mothers and babies is the primary role of maternity care. Approximately 70% of pregnant women in the United States are healthy and have normal pregnancies. That is about 3 million normal births annually.
(2) These protective and preventive methods include a commitment not to disturb the natural process. This minimal-intervention approach includes continuity of care, patience with nature, one-on-one social and emotional support, non-drug methods of pain relief and the right use of gravity. Obstetrical intervention is reserved for complications or the mother herself requests medical interventions.
(3) Physiological principles provide the safest and most cost-effective form of maternity care. According to the World Health Organization (WHO), it is the preferred standard for healthy women. WHO refers to this as the "social" model of childbirth. In the US, it is often called "family-centered" or "mother-baby father-friendly" maternity care.
Midwifery in the Modern World ~ the bell that can’t be un-rung
Midwifery is not a practice of medicine but a separate discipline arising in response to the physical, psychological and social needs of healthy childbearing women and their newborns. It is predicated on the expectation of normalcy, a respect for and trust of physiological process, and a non-interventive style which depends on specific skills and social support for the spontaneous biology of birth. This definition is to distinguish the maternity care of normal, healthy mothers – which includes treatment of minor deviations and the capacity for emergency-response by the practitioner -- from the hospital-based, high-tech practice of obstetrics, which is a surgical specialty that addresses the diseases, dysfunction and disabilities of fertility and reproduction.
Midwifery and obstetrics are distinct disciplines that deal differently with the biological events of pregnancy, labor, birth, the neonatal and postpartum period. These two disciplines exist at opposite ends of a continuum which spans from the simplest social and non-medical methods to the most complex high tech medical activities. The areas of expertise of midwifery and medicine overlap in the middle of the spectrum but they are not identical. The term 'midwifery' is correctly applied to the activities of caregivers engaged in providing normal maternity services during the spontaneous events of physiological childbearing, regardless of the educational background or status of the practitioner -- GP, family practice physician or professional midwife.
Maternity Services and Community Values
Ideally midwifery care focuses on the childbearing woman as a whole person, with social, mental, and emotional aspects of her personality that need to be taken into account. These non-physical aspects of personality bear greatly on how, when, where or even whether or not the mother will be able to labor spontaneously and give birth physiologically. The quality of the childbirth experience as defined by the mother extends beyond the moment or manner of delivery, and can affect the mother physically and physiologically for months or years, perhaps even becoming a pivotal point in her life.
The cumulative effect of the events of childbearing, in combination with other influences, extends into the mother-child relationship and can profoundly effect the quality and satisfaction in the mother’s day to day experience of parenting. Problems within the mother-child relationship can trigger a cascade of difficulties that not only negatively effect the individual family but also the stability of the community and greater societal goals. Therefore, events or caregiver activities that threaten to fracture the mother-baby bond are to be avoided and those that protect and promote it are to be pursued and supported by society. Here in lies the concept of conservative, responsible "mother-friendly" maternity care.
The principles of social or 'mother-friendly' model depend on:
-
a respect for and trust in the normal biology of pregnancy and childbirth
-
an expectation of normalcy in the progress of labor and birth
-
recognition of the mother's right to choose and control the environment for labor
-
acknowledging the mothers' right to direct her own activities, positions & postures during labor
Its practices include:
-
continuity of care
-
patience with nature
-
full-time presence of the caregiver during active labor
-
continuous one-on-one social and emotional support
-
appropriate physical and psychological privacy for the laboring woman
-
non-drug methods of pain relief such as walking, hot showers and deep water tubs
-
no arbitrary time limits as long as reasonable progress, mom & babe OK
-
vertical postures, pelvic mobility and the right use of gravity
-
maternal choice of birth position unless medical factors require otherwise
-
physiological clamping of umbilical cord -- after circulation has stopped (+/-3 minutes)
-
immediate possession and control of healthy newborn by mother and father
The
right use of gravity is a necessary part of conservative and
responsible maternity care. It naturally stimulates effective uterine
contractions, the progressive dilatation of the cervix, the
decent of the baby
through the bony pelvis and the spontaneous birth of a
healthy baby.
Non-erotic sexual nature of childbirth
Childbearing is a non-erotic facet of our normal biological sexuality. The spontaneous biology of birth is heavily influenced by psychological factors (both mental and emotional states), which are themselves an extension of normal reproductive sexuality. Labor and giving birth involves the same biological structures and similar psychological principles necessary for the normal functioning of body parts in both sexual and excretory biology. In regard to childbirth, this includes acknowledging the mother’s psychological need for privacy. The mother has the right to give or withhold consent, in regard to the participation of persons and procedures that transgress the boundaries of her body or sexual psyche. The intimate and personal nature of childbirth also requires freedom from performance pressure and arbitrary time constraints. This includes a responsibility by professional caregiver to provide the elements for success for each phase and stage of labor and birth.
A socially appropriate environment in which the mother feels unobserved and yet secure, with emotional support as necessary, is the purposeful mechanism of midwifery care which addresses the mother’s pain, her fears and privacy needs, so that labor can unfold naturally. It is also necessary to take into account the positive influence of gravity on the stimulation of labor, dilatation of the cervix and decent of the baby through the bony pelvis. Maternal mobility not only helps this process along but also diminishes the mother’s perception of pain (perhaps by stimulating endorphins).
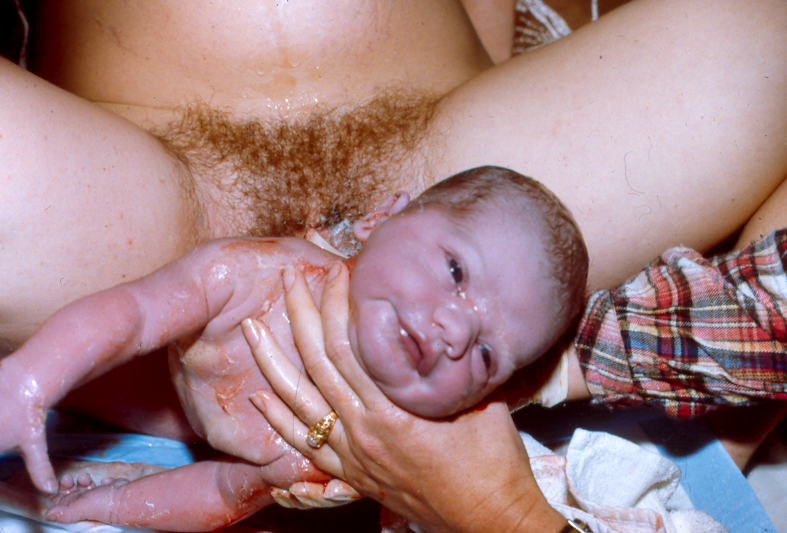
An important part of physiological management includes providing the mother with physical and psychological circumstances that facilitate the "fetal ejection reflex". This is a phenomenon was first described and named by Niles Newton, PhD and popularized by a European obstetrician, Dr. Michel Odent. It identifies Mother Nature's perfected program for the actual birth (or delivery) of the baby as physiologically similar to that of a slow-motion sneeze. When this reflexive action is unimpeded (both physically and psychologically), all the childbearing body parts work in a coordinated effort to gracefully bring about the effective expulsion of the baby with minimal pain to the mother and minimal stress to the baby. As in an actual sneeze, the normal 'taking in' direction of the body system is relaxed and reverses direction, to become a 'putting out' activity, similar to the way the upper respiratory passages reverse from breathing in to sneezing out. In this case, the abdominal muscles, the force of the uterine contraction and the unusually relaxed state of the pelvic floor all combine to quickly press the baby through, so that something which would otherwise require unnatural effort, a great deal of time and great pain, instead become a brief natural cycle occurring over the course of only 5 to 10 minutes (or less!), to the great benefit of both mother and baby.
|
|
 |
|
The Fetal Ejection Reflex -- Normal birth occurring spontaneously over the course of 60 seconds
|
|
|
|
The maternity care system
responsibility to take into account the influence of the mother’s psyche
--
riding the horse in the direction that it is going
In the absence of this quality of 'mother-friendly' support, which is the core of the traditional midwifery model of care, the mother will frequently need narcotic medication and secondarily the use of oxytocin (Pitocin) to overcome the labor retarding effects of narcotics. Additional surgical interventions of episiotomy, forceps, vacuum extraction, cesarean section often represent the failure of the maternity care system (or individuals within it) to account for the influence of the mother’s psyche in regard to the events of labor and birth.
In recognition of the highly choreographed and fine-tuned biology and psychology of spontaneous birth, the childbearing woman has a profound human right to that quality of care from her companions and her professional caregivers that does not disturb or interfere with the normal physiology of spontaneous progress in labor and birth.
| The complex interplay of the physical and the psychological are a biological verity of childbearing. Women have a right to have the maternity care provided to them be structured to address the influence of gravity and to take into account the psychological aspects of spontaneous labor and physiological birth. |
 |
The Unnatural Conflict between Midwives and Obstetricians
Most people in the United States are unaware of the highly controversial nature of midwifery and the historical tension between the professions of medicine and midwifery. There continues to be much disagreement about the contemporary relationship between physicians and midwives. At the core of the question about the modern role of midwifery is yet another question -- what is the right relationship between “modern medicine” and so-called “modern” childbearing? Has the obstetrical knowledge of the 20th century fundamentally changed the natural biological act of childbirth in the same way that medical science fundamentally changed the course of human pathology relative to illness, disease, deformity and accidental injury? Or is childbirth normally pathological, thus requiring the supervision of an obstetrician and the routine use of obstetrical interventions?
This contemporary controversy has nothing to do with the appropriate use of obstetrical medicine to treat the 30% of pregnant women who develop complications, about which there is complete agreement. Rather the question concerns using these same forms of medical interventions routinely or “prophylactically” on the 70% of healthy women with normal pregnancies.
It is the latter category – the 70% of healthy women with normal pregnancies -- that has been the traditional focus of midwifery care but which has been claimed by the obstetrical profession in the last century as their rightful patient base. In order for obstetricians in the US to enforce their preference for providing care to a healthy population, there was an extensive and largely effective campaign in the early 1900s by organized medicine to eliminate midwives in the US by various legal and legislative strategies.
In spite of this, a tiny remnant of the midwifery profession continues to practice in the United States. None-the-less, historical prejudice by the medical profession and the legal and legislative barriers that such a bias generated over the last century make it virtually impossible for midwives to take their appropriate place in the spectrum of health care services for healthy women. The greatest impact of this problem is on childbearing women, who have lost access to normal, non-interventive and psychologically-supportive maternity care and are increasingly vulnerable to unnecessary surgery as an expensive replacement for normal birth.
| For healthy women in safe surroundings, pregnancy and birth is generally successful for both mother and baby.... |
|
The scientific literature documents that physiological management – the type of non-interventive care provided by midwives for millennia – is the best and safest form of maternity care for healthy women. Midwives are "educated observers with emergency response capacity". Scientific sources also document the many serious dangers inherent in the medicalization of normal childbirth, that is, the routine use of obstetrical interventions on the 70% of healthy women with normal pregnancies.
Maternity services to healthy mothers experiencing normal pregnancies has always been provided by midwives in the home of the childbearing parents. However, most women today want and expect to labor and give birth in an institutional setting. Therefore, physiological management must be available in all settings, as it is in other parts of the world. Worldwide, the standard for maternity care is still midwifery-based, with the vast majority of all babies delivered by midwives who provide care in private homes, maternity homes and hospitals.
In those countries with the best pregnancy outcomes 70% or more of all births are attended by midwives as independent practitioners. In many European jurisdictions a midwife is required by law to be in attendance at all vaginal births (Germany, Austria, England), even when obstetrical care is being rendered. Childbirth is a natural resource of women and of society. This commonwealth, rooted for centuries in the oral tradition, has been missing from contemporary life in the United States for several decades. In the United States, midwifery and normal physiology were both stigmatized and has become marginalized, to the detriment of society.
The obstetric care policies in US depend entirely on the extreme medicalization of all childbirth. Nowhere in the government or the press does anyone question whether this is the best way or even safe. No one ever asks if the United States get its collective money’s worth from the billions and billion spent every year on interventive obstetrics for healthy women. So far the public has not been curious enough to follow the story to back in time and find out how we got here. However, it is a compelling and educational story of great importance, and understanding it is vital to making informed personal decisions and to the shaping of public policies governing our national maternity care system. So let’s revisit the early history of midwifery and find out how things veered off course, taking us to unexpected places and replacing normal maternity care in the United States with the expensive crisis-intervention mode known as obstetrics.
A Little Known Story of Great Importance
Childbearing women in the prehistoric world normally gave birth with the support of their extended families and the help of experienced older women. The original knowledge base for midwives was childbearing women themselves. Over the course of thousands of years, midwifery developed an organized body of knowledge and set of technical skills. This midwifery knowledge base precedes the modern discipline of medicine by more than 5,000 years and was the medical profession's original source of information about normal birth. The discipline of midwifery was empirically-based and organized around meeting the practical needs of laboring women, which are primarily psychological, emotional, and social. During the first five millennia's of recorded history, the normal care of midwives included ‘patience with nature’, right use of gravity and a commitment not to disturb the natural process. For healthy women in safe surroundings, pregnancy and birth was generally successful for mother and baby.
Until the 16th century, maternity care provided to childbearing women during labor and birth was uniformly and exclusively in the hands of midwives. However, not all problems associated with childbirth can be prevented by the midwifery skills of patience with nature and correct use of gravity. In a pre-scientific, pre-technological world, the normal support of midwives was not enough if the childbearing woman suffered from a serious disease, became ill during the pregnancy, the labor became abnormal or the birth was otherwise complicated. In such cases, childbirth could and often did become dangerous and midwifery alone was not enough. Prior to the development of obstetrical medicine, a vitally important piece of the system of maternity care was missing.
Birth and Birth Problems in a Pre-scientific World
As the centuries passed, more and more people abandoned safer natural environments and healthy lifestyles to migrate to big cites, where poverty and crowded unsanitary living conditions resulted in malnutrition and disease. These detrimental social forces were the result of ignorance, superstition and unnatural or abnormal situations imposed by city life in crowded urban environment. By the early Middle Ages, an increasing percentage of childbearing women were unhealthy. This resulted in many complicated pregnancies and a high mortality rate that was not the result of any deficiency in “normal” biology, but instead reflected the negative impact of civilization on health and normal childbirth. Untreated complications meant that mothers and newborn babies with serious problems could and did die. During the Middle Ages, people began to think of childbirth itself as generally dangerous. Unfortunately, they were mistaking ‘cause’ with ‘effect’. Nonetheless, it poisoned the water of public opinion and set the stage for the next four centuries of the most drastic changes in childbearing practice ever to occur in the history of the human species.
The missing piece in regard to childbirth was a reliable method of treating the increasing number of women who were experiencing serious and potentially fatal complications during childbirth. By the 16th century, the practice of medicine as a formal body of knowledge was just beginning to provide some hope to women and babies who might otherwise die or be permanently damaged by childbirth. This often meant choosing between the life of the mother and that of her baby, since the early crude methods did not allow the doctor to save both mother and baby. At first doctors were only able to intervene through the use of fetal destructive operations, later on a mother with an obstructed labor could be delivered using the newly invented obstetrical forceps.
However, inviting medical men into the birth chamber meant that 500 centuries of mutually respectful relationships between midwives and doctors were permanently changed.Initially there were serious problems with this plan, since it was a scandal (and even a crime) during the Middle Ages for male physicians to be present during labor and birth. In the beginning, medical educators had to depend on midwives and midwifery textbooks for all their information about normal birth.
Ideas soon began to percolate in the minds of doctors, and especially professors of medicine, that doctors should be more involved in the general process of childbirth. In particular, they recognized the benefits of teaching medical students about normal childbirth, since such knowledge was an important part of the ability of graduate physicians to provide care in complicated cases.
Institutionalizing Medical Education In Middle Ages Europe
The earliest versions of hospitals in Middle Ages Europe became a place for both teaching and treatment. However those first hospitals were dramatically different in form and function from our modern day acute-care medical institutions. Originally hospitals were charity hostels run by Catholic nuns to house the indigent. It turned out these hotel-like institutions were the perfect place for medical schools to teach students, as they provided a steady stream of ‘clinical material’. In a fairly short time hospitals became organized around medical education. In exchange for room, board and medical care, street people who were sick become ‘teaching cases’ for medical students.
In these charity hostels, unmarried, widowed or pregnant women abandoned by their husbands and unable to work, could find shelter in hospital maternity wards. They lived on this ‘hospitality’ for several months before their babies were born. While no money was exchanged, the human price for this free care was steep. Even in the best institutions, approximately of 1 out of 128 childbearing women died. In the typical charity hospital, the number of maternal deaths was more like 1 out of 50 and sometimes, for months at a time, as many as 1 out of 3 mothers died. One university hospital in Austria bore the unfortunate distinction of not having a single mother leave the hospital alive for four consecutive years. This reinforced the belief that childbirth itself was dangerous.
Physicians recognized early on that aggregating childbearing women together in an institutional setting resulted in a dramatic increase in maternal and infant mortality from a lethal infection known as ‘childbed fever’ or ‘puerperal sepsis’. Doctors also observed that women who gave birth at home with midwives and indigent women who gave birth on the doorsteps of the hospital, prior to admission to the maternity wards, were both remarkably free from this scourge, as were their newborn babies. And yet, inexplicably, childbearing women who labored and gave birth in the hospital often developed a virulent septicemia that caused death within 72 hours. We now know that those women became contaminated with the hemolytic streptococcal bacteria acquired from contaminated bedding, dirty instruments or the unclean hands of medical students, doctors and hospital staff.
This occurred long before there was any scientific knowledge of the role of microscopic organisms (bacteria or germs) as the cause of childbed fever and other infections. The concept of contagion between infected patients was not understood, nor the idea that deadly germs could be spread by hands, instruments or equipment contaminated by infected organic material. Before the development of the germ theory (and invention of sterile exam gloves!), these epidemics raged all across Europe on a regular basis.
Teaching Hospitals Associated with Maternal Mortality
During the 17th, 18th, and 19th centuries, maternal-infant deaths in teaching hospitals from hemolytic septicemia caused all hospitals to be thought of as places to die and therefore feared by the population. This caused a difficult public relations problem for the medical community. Early on the medical profession had recognized the great educational value and convenience of hospitals and were committed to preserving hospitals as a place of teaching and medical treatment. Despite high mortality rates for hospitalized maternity patients, the conclusion arrived at by medical profession was that hospital birth was a vital necessity in the clinical training of medical students. In 1881 an influential professor of obstetrics from the Edinburgh (Scotland) maternity hospital stated that:
“… maternity hospitals must exist ... for the clinical instruction that the medical student can receive there, and there only.”
The discovery and dissemination of the germ theory by Dr. Pasteur in 1881 brought about the widespread understanding of the role of bacteria in causing infections. This dramatically (and permanently) influenced the practice of medicine and surgery all across the world. In particular, it changed the way normal childbirth was conducted. In the late 1800s and early 1900s, the only way to prevent institutional outbreaks of puerperal sepsis was to conduct labor and birth in hospital maternity wards under conditions of surgical sterility, as a 'surgical' procedure.
Obstetrics Moves Across the Pond to the New World
By the time obstetrical medicine landed in America, the European tradition of obstetrical practice had moved far away from its roots in midwifery and physiologic process and was very entrenched in hospital-based care and a model of medical intervention. The new science of obstetrics, which was now freed from the traditional restraints of physiological management, seemed to offer unlimited possibilities to medicalize the care of all childbearing women. Obstetricians were the newly identified providers of these newly configured services.
The Law of Unintended Consequences
It is just a fluke of history that puerperal sepsis in hospitals and efforts to stop the hospital-based epidemics in 18th and 19th century Europe so influenced and defined the development of 20th century maternity care for healthy women in the United States. Unfortunately, this oddity of pre-scientific medicine continues to dominate how maternity care is provided to healthy women in the 21st century. Efforts to stop the institutional epidemics of puerperal sepsis of the 18th and 19th century morphed into a permanent epidemic of surgical interventions in normal childbirth over the course of the 20th century. Normal childbirth has been held captive in a perpetual time warp for over a hundred years.
Abnormal Medicalized Birth Becomes the Norm
The dramatic changes in maternity care for healthy women that occurred during the first three decades of the 20th century were nothing short of radical. Most of these changes were based on the assumptions that childbirth, even in healthy women, was dangerous and that the intervention of a medical professional was necessary at every birth. before the discovery of antibiotics there was also the very real fear of hemolytic septicemia in every doctor’s mind was , an unpredictable and untreatable infection of childbirth so prevalent in hospitalized women . The only prevention for puerperal sepsis was to conduct institutional birth under conditions of surgical sterility.
Thus by the early 1900s, the idea that childbirth should be conducted as a surgical procedure performed by a physician in a hospital was becoming the accepted standard, at least in the larger in urban areas. The typical physician-conducted birth usually included the use of obstetrical anesthesia and surgical instruments. Within a single generation, virtually all childbirth services were reorganized around hospitals, physicians, obstetrical interventions. Childbearing women now labored alone, in social isolation, under the influence of powerful narcotics and gave birth unconscious and separated from their family members.
By 1910, the most influential obstetricians in the United States were also promoting the routine use of episiotomy and forceps as a way to ‘save’ the mother’s pelvic floor from being damaged during childbirth. One of these doctors (Dr. Joseph DeLee) remarked that: “birth was about as normal as falling on a pitch fork". He preached that the routine use of episiotomy and forceps would also save the baby’s delicate head from being pounded on the mother's intact or "iron" perineum. Of course, the use of episiotomy and forceps to be helpful to physicians as well. It's mechanically difficult to get a baby out of a profoundly anesthetized mother who is lying on her back on a delivery table with her legs in stirrups, unconscious and unable to push effectively,. Doctors no doubt considered forceps very helpful as they allowed the doctor to accomplish the job with dispatch, thus control the situation and controlling his own time.
‘Manifest Destiny’ for Obstetrics
At this point in history, the obstetrical profession took on the mantle of being the source of all knowledge about normal reproduction and the only credible source of wisdom about proper care during childbirth. To their way of thinking, this equated to a medical version of “manifest destiny”. It was only appropriate that God and Government cede ownership rights over the biology of childbearing to the obstetrical profession, making normal childbirth the professional property of obstetricians, with all other caregivers branded as dangerous quacks and or ignorant charlatans.
“We believe it to be the duty and privilege of the medical profession of America to safeguard the health of the people; we believe it to be the duty and privilege of the obstetricians of our country to safeguard the mother and child in the dangers of childbirth.
The obstetricians are the final authority to set the standard and lead the way to safety. They alone can properly educate the medical profession, the legislators and the public.” Boston Medical and Surgical Journal, Feb. 23, 1911, page 261
To manifest their destiny as the property holders of childbirth, organized medicine had to immediately and systematically eliminate midwifery. As small sampling of comments recorded in professional journals of that demonstrate the medical campaign:
“The midwife is a relic of barbarism. In civilized countries the midwife is wrong, has always been wrong. The greatest bar to human progress has been compromise, and the midwife demands a compromise between right and wrong. All admit that the midwife is wrong.”
“The midwife has been a drag on the
progress of the science and art of obstetrics. Her existence stunts the
one and degrades the other. For many centuries she perverted obstetrics
from obtaining any standing at all among the science of medicine.”
Dr. DeLee, MD, 1915-C, p. 114
The problem was that physicians took over the practice of midwives without any idea of the philosophy, principles or techniques of the discipline of midwifery -- the physiological model of birth. They did not acknowledge the psychological and social needs of laboring women or appreciate the greater safety and other benefits afforded by respect for and strict adherence to physiological management. Most important of all, they had no understanding of the dangers introduced by medical interference and surgical interventions. Instead physicians saw the care of healthy childbearing women primarily as an educational opportunity for them to develop better skills in interventionist obstetrics. This was done by routinely using chloroform, episiotomy, forceps and manual removal of the placenta at every normal birth. Using the full range of interventive techniques routinely in all normal deliveries afforded educational opportunities for medical students to learn surgical techniques and graduate physicians to keep proficient in the use of obstetrical forceps.
Unfortunately, this obstetric interference also increased the maternal mortality rate by 15% per year and the birth injury for newborns rose by 44% during the first decades of the 20th century. However, this information was never divulged to the public.
During this same time period, obstetricians were remarkably worried about their professional image. They believed that the medical profession and the public were both mocking them.
“ ..... the ideal obstetrician is not a man-midwife, but a broad scientific man, with a surgical training, who is prepared to cope with the most serious clinical responsibilities, and at the same time is interested in extending our field of knowledge.
No longer would we hear physicians say that they cannot understand how an intelligent man can take up obstetrics, which they regard as about as serious an occupation as a terrier dog sitting before a rat hole waiting for the rat to escape." [Dr J. Whitridge Williams, M.D. 1911-B]
A part of this low self-esteem by obstetricians was the idea that attending normal births was woman's work. Remember, that virtually all physicians of that era were men and women were not even allowed to vote; thus women's work was clearly a derogatory term and and insulting, especially to a 'professional' man. . Providing care to childbearing women was classically considered to be a low-paid, low status job. Therefore it was not highly regarded nor highly compensated via a large professional fee worthy of a physician’s time and his long and expensive medical education.
“Obstetrics is held in disdain by the profession and the public. The public reasons correctly. If an uneducated women of the lowest class may practice obstetrics, is instructed by doctors and licensed by the State, it [birth attendance] certainly must require very little knowledge and skill ---surely it cannot belong the science and art of medicine. If the profession would only realize that parturition, viewed with modern eyes, is no longer a normal function, but that it has imposing pathologic dignity, the midwife would be impossible of mention.” Dr. DeLee, M.D. 1915-C; p.117
The official propaganda campaign by the obstetrical profession denigrated midwives while misrepresenting the dangers of childbirth, inflating the abilities of obstetrical intervention and ignoring or denying the dangers of such interference. The desire to eliminate midwives and replace them with obstetricians included a formal plan of attack on what was called the "midwife problem".
“How can this be done? Let us begin with the Women’s Clubs in the United States. Let us tell them of the facts we have learned here today. The Women’s Clubs in the United States are an enormous power, and they are growing more powerful in the civil and social betterment of this country. If we can disseminate among the women of our land the facts regarding obstetrics, there will rise an undeniable clamor for good obstetrics. The public will be forced to furnish the materials, and the patients [i.e. teaching cases] for the proper instruction of the doctors. They will build maternity hospitals the equal, if not the superior, of any surgical hospital.
When public opinion has thus been raised and educated regarding obstetrics, the midwife question will solve itself. With an enlightened knowledge of the importance of obstetrical art, its high ideals, the midwife will disappear, she will have become intolerable and impossible.” Dr. DeLee, M.D.1911-B
“In states where the midwife is practically unknown, it should be seen to that the Medical Practice Law excludes the possibility of midwives practicing... In states where the midwives ... are numerous, a well organized license and regulation system should control those in practice. Renew the old licenses every year and issue no new ones. Thus the midwives will gradually be excluded from practice...." [1911-C, p. 209]
“It is quite possible by strict educational requirements, by imposing certain qualifications ... and in other ways to restrict the practice of midwifery to such a degree as to amount to practical abolition. Such a method is necessarily more slow than direct abolition [but] it can be carried out ... according to the forms of law." [1911-E, p. 225]
“With sufficient repetition, perception becomes reality”
Eighty Years of Obstetrical 'Upgrades'
Having solved the “midwife problem" according to the above mentioned "forms of the law" and having dispatched with the inconvenient principles of physiology, the rest of the 20th century is just a progression of upgrades in the techniques, technologies, drugs and devices used to implement the idea that childbirth was a surgical procedure to be performed by doctors on childbearing women who lay recumbent, immobile, passive and most usually under anesthesia.
-
In 1910 the use of 'twilight sleep' (narcotics and amnesic drugs) as a pain medication for labor and chloroform anesthesia for delivery was the norm, accompanied by the routine use of episiotomy and forceps.
-
In the 1920 and 1930s the very dangerous anesthesia chloroform was upgraded to ether. Obstetrical forceps were further refined, as were the 'boogies' or small rubber balloons inserted into the cervix to pry it open as a method of induction or speeding up labor.
-
In 1940s safer anesthetics, blood typing and the new antibiotic drugs came alone as side effect of WWII, making C-sections safer and more readily used. An important part of this obstetrical ‘upgrade’ program was the rapid addition and expansion of hospital maternity wards. By the half way mark of the 20th century about 70% of babies were born in hospitals.
-
In the 1950s the first vacuum extraction devise was developed and safer anesthetics replaced the use of ether. The 1950s also got to claim Pitocin (synthetic drug to induce or speed up labor) as its major contribution. This improvement in the drugs and technology of induction replaced the use of castor oil to trigger labor and boogies to mechanically force the cervix to dilate.
-
The 1960s laid claim to the invention of electronic fetal monitors and the first obstetrical use of ultrasound. By the end of the decade the rate of hospitalization for childbirth was 99%.
-
The 1970s brought about the routine use of intravenous fluids (IVs) in labor. Putting Pitocin in the IV was a safer and better way to speed up labor and much easier for the hospital staff . This convenience lead to a big increase in the induction of labor. During the 1970s the use of 'twilight sleep' (narcotics and amnesic drugs) as a pain medication for labor and general anesthesia for delivery were replaced by the use of an epidurals for both the labor and the birth.
-
The 1980 and 1990s were mainly periods devoted to the refinement of the technology and the routine use of these techniques and equipment on each and every laboring woman.
The Obstetrical Idea of "Liberalized" L&D Policies in the 21st Century
From the perspective of the mother and her family, there have been a few important changes in the experience of childbirth during the last 80 years. Mostly of these are the result of popular childbirth education courses that teach ideas about 'natural' childbirth (originally defined as not being 'put to sleep' during the delivery) and techniques such as walking around in labor and fathers being allowed "in the delivery room". Allowing the father and family members to be present during labor and birth has simply been added into the mix of a highly medicalized process, with family members now permitted to watch the medical interventions that would be done whether or not they were present. Tight control and medicalization of the entire process is still the norm. The sheer number of medical procedures and medical devises that have become routine in the late 20th and early 21st century is staggering. At the very least, seven drugs, devises or surgical procedures is now the statistical norm and that is for healthy women.
Obstetrical Interventions in Normal Birth as a form of "Munchausen's Disease by Proxy"
While some women may now be ‘permitted’ to walk around in early labor, once things become active (or an induction is started) mothers are still required to labor in bed (74%), with electronic fetal monitor (EFM) leads severely restricting her mobility (93%). This makes it impossible to use most methods of non-drug pain relief in a hospital setting. The laboring woman is still not permitted to eat or drink and the majority will routinely have IV running (87%). The mother will be subjected to the artificial rupture of membranes (67%), Pitocin acceleration of her labor (63%), an epidural catheter placed in her spine (63%), an indwelling catheter in her bladder and taped to her leg, with a urine bag hanging from the bedrail (52%), a blood pressure cuff on her arm and pulse oximetry on her finger (63%). In most hospitals, the L&D nurses spend more time out of the room than in the room. According to one study of L&D nursing, they were out of the room 79% of the time. Of the 21% spent in the labor room, only 6% of the nurse’s time is devoted to the personalized care of the mother. [The Preventable Cesarean Section Program – Reducing C-Section Rates on the Front Line by Transforming Nursing Practice, p. 4; Outcome Management Associates; 1998, Mayri Sagady, CNM]
As for the 2nd stage of labor, the mother will push while lying on her back (71%). Although she will be exhorted to push with all her might, often turning dark purple in the face ("purple pushing"), she is still expected to be prone and passive during ‘the delivery’, in some version of a lithotomy position. The delivery is still considered to be a highly technical ‘surgical procedure’ performed by the physician on the mother. The physician will still be “scrubbed in” and wearing a long-sleeved surgical scrub gown, scrub cap, shoe covers and facemask (with splash guard), with ready access to a sterile table with an array of gleaming surgical scissors, forceps and other instrument at his fingertips. The use of some form of anesthesia is the statistical norm (63%). The mother’s participation is optional. Should she be unable to push her baby up hill and around the corner, episiotomy (36%) and forceps (or vacuum extraction) will be provided (12%). Failing that, a CS will be done (average was about 30% in 2003).
After the baby is out, a gloved hand is often inserted up into the uterus to check for placental fragments or to remove blood clots (58%). As soon as the physician puts in the last stitch, his/her official duties as an ob-gyn surgeon are completed and the mother’s “post-op” recovery will be assigned to the nursing staff. And the mother still believes, for the most part, that she could not have ‘done it’ without the physician’s advanced technical skills.
[Statistics cited above are from the October 2002 report by the Maternity Center Association “Listening to Mothers: Report of the First National US Survey of Women’s Childbearing Experiences” conducted by the Harris Interactive Polling Service. The Maternity Center Association (MCA) of New York City is a non-profit organization established in 1918]
Reconsideration of “Purple Pushing” Urged
Ob.Gyn.News; March 15, 2003 EditionPhysiology suggests that standard positioning and pushing techniques used during labor and delivery require rethinking, according to Lisa Miller, certified nurse-midwife.
Long Valsalva's maneuvers -- or "purple pushing"--- and standard supine [i.e. lying on one's back] positioning should be reconsidered. Long Valsalva pushing can adversely affect maternal hemo-dynamics, which in turn adversely affects fetal oxygenation, said Ms Miller, who also is president of Perinatal Risk Management and Education Services in Chicago.
....near-infrared spectroscopy used to evaluate fetal effects revealed that closed glottis and coached pushing efforts [when the doctor or nurse instructs the mother to hold her breath & push as long and hard as she can] led to decreased mean cerebral 02 saturation and increased mean cerebral blood volume. All Apgar scores were below 7 at one minute and below nine at five minutes.
Open-glottis pushing, on the other hand, allows the patient to exhale while bearing down and leads to minimal increase in maternal blood pressure and intra-thoracic pressure, maintained blood flow, and decreased fetal hypoxia.
REMEMBER THE FRIEDMAN CURVE -- when a patient reaches 8 cm of dilatation, remember the deceleration phase of the Friedman curve and avoid starting Pitocin as a reaction to this phase. At this phase of labor, the patient's body "takes a break" [called the "rest and be thankful phase by Shielia Kitzenger] in preparation for the hard work about to come...
But this is often misinterpreted as stalled labor.... Giving Pitocin at this stage can create fetal hyper-stimulation and can be considered "Munchausen OB," because it is basically creating an emergency in order to respond to it.... "This is indefensible", she said.
Cesarean on Steroids ~ The Obstetrical Version of the 'Preemptive Strike'
By the year 2000, the obstetrical profession had convinced itself that the elective or "maternal choice" Cesarean was the Rolls Royce of childbearing for the 21st century. This "vaginal by-pass surgery", as it is often referred to by obstetricians, was their first choice and seen as the final solution to all childbirth related problems. Coincidently with promotion of medically unnecessary C-sections, was an announcement by an ACOG task force that neither the routine use of electronic fetal monitors nor the liberal use of Cesareans over the last 30 years were able to reduce the incidence of cerebral palsy at all, which remains exactly the same as it was in the 1970s. ACOG has begun to play down the role of CS as a rescue operation for the baby, while promoting patient choice Cesarean sections as the sure fire way to prevent the damage to the mother's pelvic floor from 'purple' pushing (while on her back!) or from the use of episiotomy and forceps. ACOG is now aggressively promoting the idea of “patient-choice” Cesareans as ‘better’ and ‘safer’ choice than normal vaginal birth.
According to former ACOG president Dr. Harer:
“For the mother, the immediate risks for a cesarean section are a little higher .... Over the long term I think that the risks balance out, that there really is no big difference” (between vaginal by-pass surgery & normal birth).” [GMA interview / Dian Sawyer, 2000]
What could be called 'Cesarean on Steroids' arrived on October 31, 2003. On that date, the American College of Obstetricians and Gynecologists announced that ACOG’s Ethics Committee decided that it was professionally “ethical” for obstetricians to perform medically-unnecessary Cesareans at the “patient’s request”. It was expected that health insurers and government programs would pay for patient-choice Cesareans as a matter of course.
Modern Time, Modern Science
No mater how enthusiastic the medical profession and the public is for interventionist obstetrics and “vaginal by-pass surgery”, the science doesn’t support either one.
To get the point, one need only think of the notion that somehow kidney dialysis was being promoted as ‘better’ and safer than normal healthy kidney function or laxatives were being promoted as absolutely necessary to normal bowel function. Research published in medical journals and textbooks and records of maternal infant well-being such as birth registration and vital statistics data – all identify increased risk and unnecessary expense when drugs and surgery were compared to normal or ‘spontaneous’ birth in a healthy population. These scientific sources make it clear that, compared to the use of physiological principles, routine obstetrical interventions and normal birth conducted as a surgical procedure create unnecessary dangers for healthy women with normal pregnancies.
This means that for healthy women who are well fed, well housed, well educated and receive good prenatal care during pregnancy, the greatest realistic danger today is obstetrical over-treatment and the cascade of complications associated with routine interventions such as induction of labor, continuous use of electronic monitors, narcotics, anesthesia, episiotomy, forceps, vacuum extraction or Cesarean surgery. Scientifically speaking, this is not a controversial finding. The scientific evidence is neither lacking nor incomplete, nor is this data the subject of great methodological disputes. A mathematical formula for defining medical risk published by the Maternity Center Association of New York, shows that interventionist obstetrics for healthy women, with its high risk of Cesarean section and subsequent complications, is a highly pathological model.
The epidemic of puerperal sepsis of the 18th
and 19th century has turned into the epidemic of surgical
interventions in normal childbirth in the 20th and 21st
century.
On August 2, 2005 the Reuters news syndication headline read: “C-Sections most common US hospital procedure”. According to an article reporting on the top five most commonly performed medical and surgical procedures, the US government has identified that 1.2 million Cesarean operations are being done each year (approximately 30% of all childbirth). The total charges in 2003 for just one year’s worth of Cesarean surgery were an astounding $14.6 BILLION. The Cesarean rate in 2003 was three to six times higher than is what is biologically necessary.
Its important to remember that cesarean surgery is major abdominal surgery. None of the other four procedures that are on the government’s ‘top five’ list was for major abdominal surgery and none was done on healthy people experiencing normal biological functions. The other four procedures in the government's survey were diagnostic procedures, like endoscopies and cardiac catheterization, life-saving procedures like intubation and angioplasty.
It is even more interesting to note that the 1.3 million episiotomy was not even counted as a reportable procedure. When you combine the 1.3 million episiotomies done each year on women who have vaginal births with the 1.2 million Cesarean sections, you get a staggering total of 2.5 million women who have had serious painful surgeries performed on them in the course of a generally normal biological process. This is 66% of the approximately 4 million births that occur each year.
How Could This Have Come About?
How could a smart country like ours, with so many resources, one that is exceptionally good in so many areas of education, science, technology, and ‘medical miracles’, etc., have the greatest realistic danger faced by its healthy and wealthy women be obstetrical over-treatment and the cascade of complications associated with their use?
The answer is straightforward and right out of the history books. When the scientific principles of physiological management are rejected by medical educators and abandoned by practicing physicians, when midwifery is publicly denigrated by organized medicine and midwives criminalized at the request of the obstetrical profession, when childbearing women are isolated from the family and narcotized during labor, anesthetized and delivered surgically, it results in the total erasure of all institutional and cultural memory of normal birth.
Under those circumstances, neither citizens nor the decision-makers in society and government have any direct experience upon which to base informed decisions. As a result, the public no longer knows anything about the biology of birth and must believe whatever the “experts” tells us. In the place of thousands of years of cultural memory and hundreds of years of institutional memory (and the sound science upon which the physiological childbirth rests in modern times), misinformation and misleading claims have taken over. These false claims have been coupled with a lack of true informed consent for the use of interventionist obstetrics on healthy women with normal pregnancies, leading to an epidemic of obstetrical interference in the normal births of healthy women.
The problem is that physicians are the natural spokespersons for the scientific discipline of medicine. This places a societal burden of candor and accuracy on doctors by virtue of their advanced education and their license to practice medicine and creates a higher standard of conduct than mere recitation of personal preference or professional self-promotion.
As amply demonstrated by the literature, many of those with a doctorate in obstetrics are not living up to their obligation to speak and act on the best scientific evidence. The problem is that physicians, by virtue of their advanced education and their license to practice medicine, have become the natural spokespersons for the scientific discipline of medicine. This places a societal burden of candor and accuracy on doctors and creates a higher standard of conduct than mere recitation of personal preference or professional self-promotion. Even the American Medical Association argues that a licensed physician has a legal or 'due diligence' obligation to provide "honest, complete, and impartial" information in regard to 'expert testimony' as provided in malpractice cases. Is it not logical that this same ethical principle would apply to obstetrical advice about treatment options and management style for normal birth? The very fact that physicians are holders of a doctorate in the science of medicine (equivalent to a PhD) gives the public every good reason to believe that formal statements made by physicians about matters of health, safety and medical care are unbiased, scientifically-based and factually correct. This would include a duty to communicate only scientifically valid information in a public forum unless such statements are identified as merely a personal or political opinion.
When put all together, this short list encapsulates the history of how the normal biology of reproduction was misappropriated by the obstetrical profession in 20th century America. It explains why and how the obstetrical profession came to eliminate normal birth and replace it with dangerous surgery, while marketing Cesarean section as the newer, better 21st century technology and the safer choice.
The only thing it doesn’t account for is how the entire population of the United States can believe this preposterous story.
What went wrong?
Dr. P.W. van Peyma, a physician who had 40 years experience working with midwives in New York State, makes the point most succinctly in a 1915 criticism of efforts by organized medicine to eliminate the care of midwives and the plan to substitute obstetrical care in place of midwifery and his deep concern over the escalating rate of operative deliveries by obstetricians:
"The present wave of operative interference is disastrous. ...The situation would not be improved by turning (the patients of midwives) into the hands of such medical men ..... The essential difference between a midwife and a physician is that (physicians) are free to hasten delivery by means of forceps, version, etc. … Time is an element of first importance in labor, and the midwife is more inclined to give this than is the average physician.”